Recent News from Dr. Galante
Dr. Galante is here to share some exciting news! There has never been a time in history when the chiropractic profession has received more positive press than in the last 24 months. Medical journals confirm: seeing a chiropractor beats opioids and back surgery.
Medical Journals Confirm: Seeing a Chiropractor Beats Opioids and Back Surgery
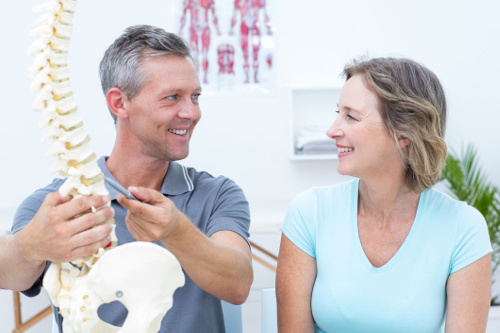
Over 100 people a day die from opioid overdoses. One of the leading causes for opioid prescriptions is lower back pain, something a chiropractor can treat very well. This is why medical journals and healthcare experts now recommend seeing a chiropractor like Dr. Galante first before you try other treatments. Our own Dr. Galante highly recommends this path of action as well!
Dr. Galante’s Here to Tell You That Chiropractic Beats Back Surgery, Opioids, and Steroid Injections
Dr. Galante is here to share some breaking news: studies show lower back surgery may not be the “cure-all” that surgeons would lead you to think. Believe it or not, most lower back pain can be treated without surgical intervention.
Epidural steroid injections and other invasive treatments can be painful. Worse, they sometimes yield no, or only partial, benefits. One study showed the long-term success rate for these types of treatments to be only 15%.
Physical therapy may be too difficult for some back-pain patients. Patients with high levels of inflammation and serious back conditions like sciatica, disc herniation or arthritis might find physical therapy especially challenging. For these patients, studies show that seeing a chiropractor may be more effective than physical therapy.
Lower back pain remains one of the most expensive maladies in our country. That includes disc herniations, sciatica, stenosis, degenerative disc disease, sprain/strain injuries, sacroiliac syndrome, spondylolisthesis and more. It’s estimated that people spend $80-100 billion per year on low back pain in America. That’s THREE times more than what’s spent on breast cancer.
Low back pain is the leading cause of disability in our country and worldwide, truly an epidemic.
Did you ever hear someone say, “I had low back pain and then it went away.” That is not a good thing. That means they will never address the problem with proper exam, imaging, and treatment. Why is that bad? Low back pain has a 60% recurrence rate in one year and a 94% recurrence rate in 4 years. Low back pain does not “go away,” it lays quietly for a while until it decides to show up again.

Dr. Galante Shares: Good Press for Chiropractors, Bad Press for Opioids
Lets take a look at some chiropractor love in the press:
Harvard Health Letter a newsletter published by Harvard Medical School, in the November, 2017 edition starts out like this:
“Low back pain is one of the most common complaints on the planet. Chiropractors use posture exercises and hands-on spinal manipulation to relieve back pain, improve function, and help the body heal itself. They often work with other doctors, and they can prescribe diet, exercise, and stretching programs. “A well-trained chiropractor will sort out whether you should be in their care or the care of a physical therapist or medical doctor,” Dr. Kowalski explains.
The article goes on to say: “In most cases, you won’t need to see a specialist,” says Dr. Robert Shmerling, a rheumatologist at Harvard-affiliated Beth Israel Deaconess Medical Center. “A referral to a specialist makes sense when conservative measures have failed to address your back pain, symptoms aren’t improving or are getting worse, or there’s a clinical suspicion that surgery might be needed,” says Dr. Shmerling.
This is what chiropractors like Dr. Galante have known for decades. Over the first two to four weeks of treatment, patients are expected to see a 25-50% improvement in their symptoms. If their pain isn’t alleviated in this time frame, then advanced imaging and specialist referrals are considered.
An article in To Your Health newsletter, “Why Opioids Became an Epidemic and How Chiropractors Can Solve It.”
U.S. Senate Homeland Security & Governmental Affairs Committee inked a report titled, “Fueling an Epidemic: Exposing the Financial Ties Between Opioid Manufacturers and Third-Party Advocacy Groups.” This report exposes just a few of the corrupt ways drug companies used their money to advance their pro-opioid agenda that now kills over 100 people a day! Read for yourself:

The article continues:
Why Chiropractic Matters Now More Than Ever
If there’s any possible upside to the opioid epidemic, it’s that the crisis is now front and center. Policy- and practice-level changes are being implemented to replace prescription pain-relief medications such as opioids with safer alternatives as the first option – including chiropractic care. Of course, chiropractors have always practiced drug-less care and provided effective, natural pain relief for a variety of conditions, including low back pain.
JAMA – Journal of the American Medical Association, March 6, 2018
JAMA is a well-respected journal and they have done some fascinating research. They asked the question, “Do opioids work better than non-opioid medications?” That question has never been asked, never been studied, millions and millions of prescriptions given out to countless Americans and your doctor does not even know if it works!
Findings: In this randomized clinical trial that included 240 patients, the use of opioid vs non-opioid medication therapy did not result in significantly better pain-related function over 12 months (3.4 vs 3.3 points on an 11-point scale at 12 months, respectively).
And now we know the answer to their question: NO!
JAMA goes on to say:
Conclusions and Relevance Treatment with opioids was not superior to treatment with non-opioid medications for improving pain-related function over 12 months. Results do not support initiation of opioid therapy for moderate to severe chronic back pain or hip or knee osteoarthritis pain.
According to this study we may not even need opioids, we certainly do not need them as a first option.
The Lancet, another well-respected journal, did a three-paper series on the worldwide problem of low back pain.
Paper #1: “Globally, years lived with disability caused by low back pain increased by 54% between 1990 and 2015, mainly because of population increase and aging, with the largest increase seen in low-income and middle-income countries. Low back pain is now the leading cause of disability worldwide. “
Lancet states medications, injections, and surgery should NOT be a preferred or first-line treatment option. They should only be applicable for people who have exhausted conservative care options.
Paper #2: “For nearly all people with low back pain, it isn’t possible to identify a specific cause. Only a small proportion of people have a well understood pathological cause—eg, a vertebral fracture, malignancy, or infection. People with physically demanding jobs, physical and mental comorbidities, smokers, and obese individuals are at greatest risk of reporting low back pain. Most people with new episodes of low back pain recover quickly; however, recurrence is common and in a small proportion of people, low back pain becomes persistent and disabling. Disability and costs attributed to low back pain are projected to increase in coming decades.”
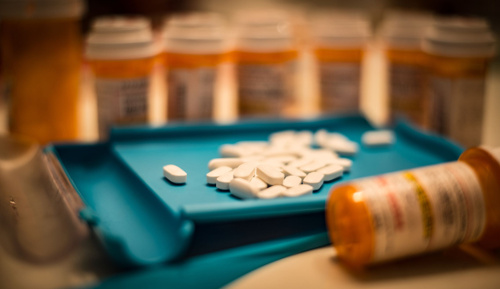
No known cause, leading cause of disability, recurrence is common, can become disabling and disability and costs are expected to increase in the future…that is the low back pain epidemic. Whatever medicine has been doing for low back pain it is not working, we need a better answer.
Paper #3: Is a “call to action” and basically gives ideas on how to improve this problem on a worldwide basis. They advocate for an update of the clinical pathways and a collaborative model of care with the inclusion of options like chiropractic care.
Good Morning America, March 2018
Good Morning America aired a piece about low back pain after new research published in The Lancet surfaced. The segment encouraged non-pharmacological pain management prior to resorting to prescription opioids. Among the suggestions were staying active, applying heat, and spinal manipulation. These are treatments that 94 percent of chiropractors perform to alleviate lower back pain.
Blue Cross Blue Shield Association, March 29, 2018
The Blue Cross Blue Shield Association (BCBSA) National Council of Physician and Pharmacist Executives (NCPE) at its March meeting adopted a professional standard that opioids should not be prescribed as first or second lines of pain therapy in most clinical situations.
The committee that includes medical officers and pharmacy experts from Blue Cross and Blue Shield (BCBS) companies around the nation, and its recommendations aligns with recent CDC (Center for Disease Control) low back pain guidelines.
1 in 5 of BCBS commercially insured members filled at least one opioid prescription in 2015, according to a BCBSA study.
Dr. Trent Haywood, chief medical officer for BCBSA, “Due to the lack of evidence combined with significant potential for harm, we believe professional standards require that BCBS members are given alternative options to opioids in most clinical situations, we will work with medical professionals to ensure BCBS members are routinely provided alternatives to opioids through a mutual decision made inside the doctor’s office.”
An article in To Your Health newsletter, April, 2018, titled, “Pain Pills Don’t Go Away After Back Surgery.”
Shockingly: Among nearly 2,500 adult patients who underwent lumbar fusion surgery, almost half used opioids long term prior to surgery. Of those pre-surgical users, a whopping 77 percent continued to use their opioid medication long after surgery. 14 percent continued use on a periodic basis. Only 9 percent discontinued opioid use or used them post-surgically for only a brief period of time. Of the 77 percent who continued long-term use, 45 percent actually had their dosage increased following surgery. To top it all off, 13 percent of patients who did not use opioids before surgery became long-term users after the procedure.

So, is spine surgery failing to take away the pain, or is opioid use a hard habit to break? Both probably deserve equal blame.
How would you like to go in for the “cure-all” surgery and come out worse, taking more opioids than prior to surgery?
Alternative treatments for new patients with chronic pain helping with opioid decline, May 6, 2018, in West Virginia, A new law sets limits on opioid prescriptions and mandates that health-care practitioners prescribe or recommend physical therapy, occupational therapy, acupuncture, massage therapy and chiropractic care for new patients with conditions that cause chronic pain.
In Prevention Magazine, May, 2018, Chiropractic care was featured as the first choice in the article, “11 Solutions for Sciatica.” The article showed that 60% of patients with sciatica who tried spinal manipulation experienced the same pain relief as patients who had surgery
A Common Theme: See a Chiropractor Like Dr. Galante First
Like Dr. Galante did, you can see these studies and press releases are all basically saying the same thing when you start reading them.
Limit your over-the-counter or prescription medications, avoid opioids, avoid invasive procedures like surgery unless absolutely necessary. Try conservative measures like spinal manipulation, massage and exercise first.
Experts from Harvard, The Lancet, and many others are making the same recommendations chiropractors like Dr. Galante have been for decades. After years of being misunderstood, the chiropractic profession is finally receiving endorsements from the rest of the medical community.
When you come in as a new patient we will do a consultation, examination, and perform any necessary diagnostic imaging. We only accept your case if we feel there is a good chance of getting well. We aim for a 25-50% improvement in the first 2-4 weeks of care. If that’s not possible, then we consider advanced imaging and orthopedic referral. You will be counseled in good nutrition and will NEVER receive an opioid medication from myself or any other chiropractor.
Choose chiropractic first, the medical doctors and surgeon recommend it now!
